The demand for mental health support is growing much faster than providers can keep up. Clinics everywhere are feeling the pressure, long waiting lists, mountains of paperwork, a high number of missed appointments, and a workforce that is reaching a breaking point with burnout. It’s no longer just about providing great care; it’s about figuring out how to run a practice efficiently enough to actually help everyone who needs it.
This is where AI and automation are starting to make a real difference. It’s not about replacing therapists or turning mental health into a cold algorithm. Instead, it’s about clearing away the daily administrative headaches that weigh clinicians down, giving them the breathing room to focus on the deeply human work that only practitioners can do.
The Real Problem: Operational Inefficiency in Mental Healthcare
Mental health organizations today aren’t struggling because their clinicians lack expertise. They’re struggling because they are operationally exhausted, trapped in systems never built to handle the sheer volume and complexity of modern behavioral health needs.
Right now, over 122 million Americans live in areas where mental health support is nearly impossible to find. Globally, the average wait time for an appointment is a staggering 70 days. These aren’t just numbers on a page; they represent people in crisis waiting for a lifeline, and clinicians working themselves to the bone trying to bridge a gap that keeps getting wider.
The real cause behind this pile of work is often “the system” itself. We see it breaking down in four major ways:
- The “Paperwork” Wall: Intake is often a nightmare of PDFs and manual data entry. Verifying insurance still feels like a relic of the 90s, requiring endless phone calls and portal hopping. While staff are stuck doing data entry, patients are stuck in the waiting room.
- The Burnout Crisis: Half of all behavioral health providers are facing serious burnout. Surprisingly, the stress isn’t coming from the patients; it’s coming from the paperwork. Between SOAP (Subjective, Objective, Assessment, Plan) notes, CPT (Current Procedural Terminology) codes, and the constant battle for prior authorizations, many therapists are spending as much time talking to a screen as they are talking to a human being.
- The Silence Between Sessions: It’s incredibly common for patients to drop out after just one or two visits. Yet, most practices have no way to catch this. Without a system to flag early disengagement, people quietly slip through the cracks of the healthcare system with no one to pull them back in.
- The Scalability Trap: If every single step, from the first call to the final bill, requires manual labor, growth becomes impossible. In a world where we already don’t have enough providers, a model that relies solely on adding more “human hours” simply cannot keep up with the world’s needs.
AI in Mental Healthcare: A Workflow Layer, Not Just a Tool
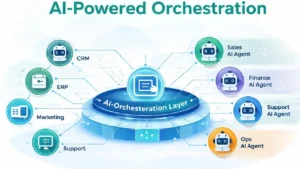
The biggest shift in how we think about AI in mental health is this: AI isn’t a product you buy; it’s a layer you add to how you already work.
If you have a standalone AI tool that summarizes notes but doesn’t “talk” to your electronic health records (EHR), you don’t have a solution; you just have another app to manage. The organizations truly making progress aren’t just using AI in small, isolated corners. They’re integrating it into the entire patient journey, from the first intake call all the way to the final bill.
Think of AI as the “brain” beneath the surface of your clinic’s daily tasks. It takes over the repetitive, data-heavy, rule-based chores that don’t actually require a human’s clinical judgment. It makes sure the right information pops up exactly when a doctor needs it. Essentially, it mends the broken links in scheduling, documentation, and billing that usually slow everything down.
So, the real question shouldn’t be, “Which AI tool should we buy next?” Instead, it should be: “Where is the most friction in our day-to-day work, and how can we use automation to fix that system for good?”
High-Impact Use Cases of AI and Automation
AI and automation create the most value when applied to specific, high-friction points in the care journey. Instead of broad, abstract improvements, their impact shows up in everyday workflows that clinicians and staff deal with constantly.
Here are some of the most practical, high-impact use cases where organizations are already seeing measurable results.
Smart Intake and Triage
Instead of handing a new patient a clipboard full of messy paperwork, modern systems send a simple digital link before the first visit. Patients can fill out their history, screening tools, and insurance info whenever they have a free moment. Behind the scenes, the AI checks their insurance instantly and updates their file. It even flags high-risk cases so the clinician knows exactly who needs urgent attention before they even open the door.
| The payoff: Front-desk stress drops by 80%, manual data entry basically disappears, and therapists walk into sessions feeling prepared rather than playing catch-up. |
Fixing the Scheduling Headache
No-shows are a massive drain, costing the U.S. healthcare system billions and leaving therapists with empty gaps in their day. AI looks at past patterns to predict who might miss an appointment and sends out friendly, automated reminders via text or email. Patients can confirm or reschedule with a quick tap, and if a spot opens up, the system automatically pulls someone in from the waitlist.
| The payoff: Real-world results show no-show rates dropping by nearly 40%, meaning more people get help and the clinic runs much more smoothly. |
Actually Enjoying the Work (Minus the Notes)
Many therapists see eight patients a day and then spend three hours writing notes. It’s the fastest route to burnout. “Ambient AI” tools can now listen in on a session (with the patient’s okay) and draft the clinical notes automatically.
| The payoff: Clinicians are saving anywhere from 30 minutes to two hours every single day. Instead of taking work home or staring at a screen all evening, they can actually finish their notes during office hours and focus on the person sitting in front of them. |
Staying Connected Between Visits
Therapy shouldn’t just be a one-hour conversation that happens once every two weeks. AI platforms can send quick check-ins or mood trackers to patients between sessions. If someone’s mental health scores start to slip or if they stop responding entirely, the system alerts the care team right away.
| The payoff: It turns a series of disconnected appointments into a continuous journey of care. It helps keep patients from dropping out and gives therapists a much clearer picture of how their patients are doing in the “real world.” |
Taking the Stress Out of Billing
Mental health billing is notoriously complicated; psychiatrists actually deal with the highest claim denial rates in medicine. AI can step in to verify insurance eligibility before the patient even arrives and suggest the right billing codes based on the session notes. It “scrubs” claims for errors before they’re sent out to make sure they don’t get rejected.
| The payoff: It stops the “leaking” of revenue from simple clerical errors and ensures the practice stays financially healthy without the constant headache of chasing down denied claims. |
Compliance, Privacy, and Ethical Considerations
AI in mental healthcare operates in one of the most sensitive data environments in all of healthcare, and compliance is not optional; it is the foundation on which any deployment must be built.
Any AI vendor processing protected health information (PHI) must operate under a signed Business Associate Agreement (BAA). In January 2025, HHS proposed the first major update to the HIPAA Security Rule in over 20 years, introducing stricter requirements for encryption, risk management, and system resilience. Vendor evaluation must be conducted against these updated standards, not legacy benchmarks.
Patients must give explicit, informed consent to AI-assisted documentation, particularly ambient scribing tools that operate during clinical sessions. AI systems must never make unsupervised clinical decisions. Every AI-generated output, whether a note, a risk flag, or a billing code, requires human review and sign-off. The clinician remains the responsible party.
Algorithmic bias is also a genuine risk. AI tools trained on historical healthcare data may reflect existing inequities in care access or treatment outcomes. Organizations have a responsibility to evaluate the assumptions embedded in the tools they deploy, particularly when those tools influence triage decisions or risk stratification.
Organizations that treat compliance as a checkbox rather than a governance commitment expose themselves legally, ethically, and reputationally. The standard for AI in mental healthcare must be higher than in less sensitive clinical domains.
The Before and After: A Real-World Workflow Shift
To see how this actually changes things, let’s look at the “old way” versus the “new way.”
The Old Way: A Cycle of Friction
A new patient calls and leaves a voicemail. A staff member calls them back the next day, emails a PDF, and then spends an hour manually typing that patient’s handwritten info into the computer. They spend another 20 minutes on hold with an insurance company just to verify coverage.
By the time the session starts, the therapist is looking at a messy, incomplete file. After the patient leaves, the therapist spends 30 minutes trying to remember the details for a SOAP note. Days later, a billing person guesses the codes, the claim gets rejected for a typo, and the practice loses $180, plus the hours spent trying to fix the mistake.
The New Way: Focus on the Person
The patient signs up on their own time, maybe at 9 PM after the kids are in bed. They get a digital link immediately, fill out their assessments, and their insurance is verified instantly. No one has to type a single thing into the system; it’s already there.
The therapist walks into that first meeting with a clear, full picture of the patient. During the session, an AI assistant quietly handles the notes, which the therapist reviews and approves in minutes. The right billing codes are suggested automatically, the claim is checked for errors, and it’s sent off the same day.
Between appointments, the system sends a quick check-in to see how the patient is doing. If their mood drops, the therapist gets a heads-up so they can prepare for the next visit.
| Takeaway: The “human” part, the conversation, the connection, and the clinical expertise, haven’t changed at all. AI isn’t replacing the therapist; it’s just clearing away the “busy work” that gets in the way of the care. |
Measuring ROI: Why This Matters for Mental Health Organizations
Investing in AI and automation isn’t just about “cool tech”; it’s about the health of the practice itself. We see the real returns in four main areas:
- Stopping “Leaky” Revenue: Many practices lose up to 20% of their income simply because of billing errors. Automation cleans up these claims before they’re sent out, meaning you start seeing that recovered money almost immediately, often within the first month.
- Giving Time Back to Clinicians: If you can save a therapist 60 minutes of paperwork every single day, you’ve just handed them back five hours a week. That’s time they can use to see more patients who are waiting for help, or, just as importantly, time they can use to actually go home on time and recharge.
- Filling Empty Gaps: A 30% drop in no-shows might sound small, but for a busy practice, it can mean recovering over $200,000 a year. It’s about making sure the schedule stays full and the doors stay open.
- Keeping Great People: It can cost $50,000 just to find and train one new clinician. By stripping away the administrative “grunt work” that leads to burnout, you’re investing in your team’s well-being. Keeping your current staff happy and focused on their patients is one of the smartest financial moves a practice can make.
A Practical Implementation Roadmap: How to Implement Automation in Healthcare?
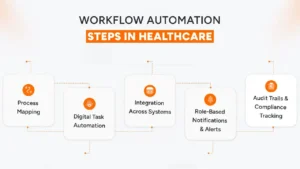
Understanding the potential of AI is only the first step. The real impact comes from how thoughtfully it is implemented within existing workflows. Rather than large-scale implementation at once, successful organizations take a phased, operational approach that minimizes disruption while delivering measurable value early.
| Phase | Actionable Focus |
| 1. Identify Friction Points | Audit daily workflows to pinpoint administrative bottlenecks (intake, scheduling, documentation, billing) where clinicians lose the most time. Prioritize high-volume, repeatable tasks. |
| 2. Start with Low-Risk Automation | Deploy AI in non-clinical areas first, such as scheduling optimization, automated reminders, and eligibility verification, to build internal confidence and quick ROI. |
| 3. Integrate with Core Systems | Ensure AI tools integrate seamlessly with EHRs and billing platforms to avoid fragmented workflows and duplicate effort. Interoperability is critical for scale. |
| 4. Introduce Clinical Support | Gradually implement ambient documentation and clinical decision support tools with strict human-in-the-loop validation and consent protocols. |
| 5. Train and Align Teams | Invest in staff onboarding, emphasizing how AI reduces workload rather than replaces roles. Adoption depends more on trust than technology. |
| 6. Measure, Iterate, Scale | Track KPIs like no-show rates, documentation time, claim denials, and patient retention. Use these insights to refine workflows and expand implementation. |
Looking Ahead: The Future of Mental HealthCare Operations
The market for AI in mental health is expected to skyrocket, growing from around $1.8 billion today to nearly $28 billion by 2035. This isn’t just about “hype”; it’s a reflection of how badly we need better systems and how much potential there is for technology to help responsibly.
The organizations that will come out on top are the ones starting to build their foundations now. By being early adopters, they’ll have a few years of solid data by 2027. That data is a powerful tool; it helps them negotiate better contracts with insurance companies, prove the quality of their care, and, most importantly, attract the best clinical talent. After all, the best therapists want to work in places where they can actually be therapists, not full-time data entry clerks.
Final Thought
A therapist sitting across from someone in distress brings something no algorithm can ever touch: true clinical judgment, deep empathy, and a genuine human presence. That connection is the heart of mental healthcare, and we have to protect it at all costs.
What AI and automation do is protect that relationship from everything else: the endless paperwork, the scheduling headaches, the insurance battles, and the SOAP notes written at midnight. These are the weights that wear therapists down, lead to burnout, and ultimately limit how many people they can help.
AI doesn’t make a therapist “better” at their craft. Instead, it makes the world around the therapist better. It creates an environment where more patients can get help faster, stay in treatment longer, and get the consistent care they deserve.
For organizations looking to operationalize these capabilities at scale, partnering with teams experienced in AI-powered healthcare app development services can help ensure seamless integration, compliance, and long-term success. We at Simpalm have worked across healthcare applications and have industry experience of 15+ years. We excel at building user-friendly mobile applications and platforms that are HIPAA-compliant, support AI-driven automation, and offer patient-focused digital experiences. As the healthcare solutions modernize, this isn’t just a technology decision. It’s a commitment to building a system that puts people first.